At an intensive care unit for infants in a Bangalore hospital, a nurse gently unhooks an impossibly tiny and fragile infant from a respirator. As she turns the baby over and softly massages lotion on its back, she says, “Many premature babies have under-developed lungs, which is why they need help breathing. Their skin is also very thin and gets very dry, so it needs extra care.”
Infants born before the 37th week of pregnancy are considered premature babies. Apart from breathing and skin issues right after birth, they are at high risk of hearing and sight problems, delayed brain development and gastrointestinal complications. Pre-term birth is the most common cause of infant deaths in the world, with about 1 million babies dying out of the 15 million that are born.
Although the cause of pre-term birth is often not known, bacterial infections of the vagina and uterus are often suspected. Now, a team of Indian scientists have shown how Group B Streptococci (GBS) — bacteria frequently associated with premature deliveries — could be causing pre-term births. These bacteria produce packets of virulent proteins that inflame and weaken uterine and fetal membranes, leading to premature birth.
One of the most common causes of pre-term birth is a condition called chorio-amnionitis, where the fetal membranes in the uterus are inflamed. In about 20 – 30% of such cases, bacteria are found to be the culprits, and a strong correlation between GBS infection and chorio-amnionitis has been found.
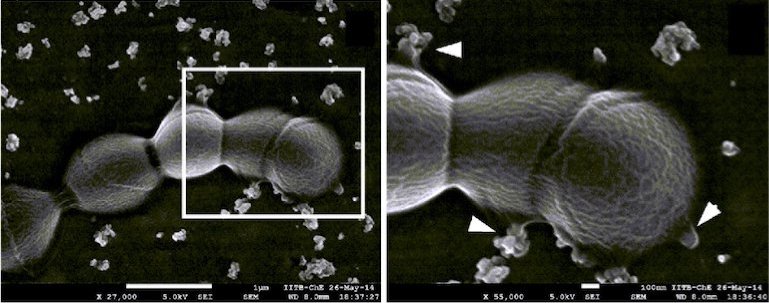
However, in a majority of these cases, no bacteria are found in the fetal membranes or in the amniotic fluid during pregnancy. “This got us thinking. What if a bacterium in the lower reproductive tract is secreting some factors that are causing this inflammation?” says Anirban Banerjee from IIT Mumbai. “When we did experiments, we found that GBS produce structures called membrane vesicles or MVs that are loaded with virulence factors,” he adds.
Using mice as experimental models, Banerjee’s team in collaboration with Deepak Modi from National Institute for Research in Reproductive Health (NIRRH), Mumbai, have shown that the MVs produced by GBS bacteria in the lower genital tract can travel up into the uterus. Their experiments also reveal that the MVs are loaded with an enzyme called collagenase. Collagenase weakens the mechanical strength of fetal membranes, making them less stiff and more prone to rupture. Furthermore, MVs can initiate an immune response bearing the hallmarks of chorio-amnionitis with the recruitment of immune cells and widespread inflammation. Finally, injecting MVs into the uterus of pregnant mice caused pre-term birth and the delivery of premature and often deformed babies.
A major drawback of the current study, however, is the use of mice as a model system admits Banerjee. Although rhesus monkeys would have been better models, these experiments are expensive and Banerjee has had no success in obtaining funding for his work on GBS in India.
“India has one of the highest rates of neonatal sepsis and infant mortality in the world. But I’m not sure at this point of time, how many can be attributed to Group B Streptococcal infections. And unfortunately, there is no epidemiological data,” says Banerjee. “Most Indians, even doctors, seem unaware of this bacterium,” he adds. Globally, the most common cause of neonatal meningitis and sepsis — both life-threatening conditions in infants — is GBS. Despite this, research on GBS in India has been lagging.
The only known treatment to prevent GBS infections in infants is to provide intravenous antibiotics to mothers during delivery. There are no available vaccines as of now. In October this year, however, the biopharmaceutical giant Pfizer has been awarded a Bill & Melinda Gates Foundation grant to test their candidate vaccine against GBS.
Since MVs from other bacteria such as the food poisoning agent Clostridium perfringens can be used to induce immunity, Banerjee hopes to use GBS MVs to design vaccines. “This is an important field of research and we hope to pursue it in the future,” says Banerjee.