Early diagnosis is critical for the effective treatment of cancer and there has been a strong push for non-invasive and rapid techniques to detect malignant cells. In a new study, researchers from S N Bose National Centre for Basic Sciences, Saha Institute of Nuclear Physics, and Bose Institute, Kolkata have come up with a method to identify colon cancer cells using a biomarker that can be detected in low levels in bodily fluids.
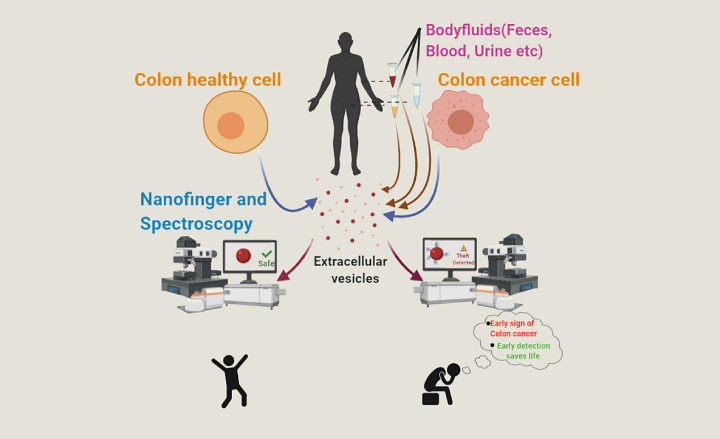
Cancerous cells secrete certain compounds into the inter-cellular region that make their way into bodily fluids like blood, urine, or faeces. Scientists are actively researching such red flags in bodily fluids which can indicate if a tumour is turning malignant. This screening process, called ‘fluid biopsy’, is set to transform cancer diagnosis from an invasive to a non-invasive method.
In one such attempt, Tatini Rakshit and her team from S N Bose National Centre for Basic Sciences, Kolkata, collaborated with researchers from two other Kolkata-based institutes — Saha Institute of Nuclear Physics (SINP) and Bose Institute — to identify that a compound called hyaluronan has the potential to be a biomarker for colon cancer. Colon cancer is the malignancy of the intestines and has a high mortality rate.
Cells often secrete fat-covered sac-like pouches called extracellular vesicles which contain cellular components like proteins, sugars, or nucleic acid fragments. These cargo-laden vesicles released from the cells can act as messengers to communicate with other cells.
Extracellular vesicles coated with hyaluronan are abundantly generated by our bone marrow stem cells. Hyaluronan is a sugar (carbohydrate) molecule that helps in regenerating damaged tissue and keeps the joints well-lubricated. It also has multiple other biological functions, including the regulation of cell growth.
Recent studies indicate that large amounts of hyaluronan are present around tumour cells. This might be because cancer cells secrete hyaluronan-coated vesicles that carry signals for cell invasion and malignant growth. As hyaluronan is easily detectable in body fluids like blood and urine, the sugar molecule has garnered attention from researchers as a potential biomarker for cancer.
“Although hyaluronan’s importance is recognised, currently it is technically challenging to identify with certainty and differentiate it from healthy cells in blood plasma,” says Arun Chattopadhyay, professor at Indian Institute of Technology, Guwahati. He was not involved in this study.
Rakshit’s team has made progress in this direction by devising a novel biophysical technique to target and screen individual cancer-based vesicles. To do this, they used a high-resolution powerful modern microscope called Atomic Force Microscope to hunt for vesicles. After identifying them, the hyaluronan coating on the vesicles is analysed by a process called Atomic Force Spectroscopy which evaluates their response to specific laser radiation. This two-step procedure detects and identifies the biomarker and ascertains its levels on a small number of vesicles. The technique can achieve this even in the early stages of the disease when hyaluronan concentration is very low.
The study reveals that the cancer cells release at least twice more vesicles than healthy colon cells, and are also morphologically different from them. “We discovered that the colon cancer cell vesicles were heavily coated with hyaluronan compared to their healthy counterparts,” says Rakshit.
To ensure that hyaluronan is accurately identified and quantified on cancer-cell vesicles, the researchers exploited a nano-sized probe of the Atomic Force Microscope. The nano-probe has a long arm with a pointed tip that moves up, down, and across the sample. The team modified the tip of the probe by attaching a specific protein molecule that can recognise hyaluronan. When this altered tip was tested on lab culture samples containing colon cancer cells, they found that the tip effectively locked with hyaluronan-coated cancer vesicles.
After the probe precisely latched on to cancer vesicles, rigorous spectroscopy analysis was used to assess the density of hyaluronan. With this combined set-up, the researchers designed an ultra-sensitive tool, labelling it a ‘nano-finger’ that could point to each vesicle, screen it, and evaluate it for the biomarker. The study also established that this novel adaptation yields highly reproducible results.
Rakshit says that the data from their research strongly suggests that hyaluronan-enriched extracellular vesicles can be used as biomarkers to detect early-stage colon cancer. The team is scaling up the study to test the technique on clinical fluid samples.
Besides, the team believes that with suitable tweaks, this technique has the potential to be a versatile tool. By changing the binding protein at the nano-tip, the nano-finger can recognise biomarkers from ovarian, breast and prostate cancer vesicles collected from body fluids. They are now working on breast cancer protein biomarkers.
“The novel technique is a commendable one,” says Chattopadhyay. “Further tests to surpass hurdles like variations in the samples and overlap with other biomolecules will establish the efficacy of the method, and to become a viable alternative to the current screening techniques,” he concludes.