Gallbladder cancer has a high rate of incidence in Indian populations and a heavy mortality rate. Now, researchers from ACTREC, Mumbai, have pinpointed a pair of genetic mutations in gallbladder cancer patients, which may serve as potential drug targets for treatment.
In a recent study, researchers led by Amit Dutt from the Tata Memorial Centre, ACTREC, Mumbai, have identified new potential genetic drug targets for gallbladder cancer by profiling mutations in Indian patients. These results may point a way towards personalized treatment for gallbladder cancer, a form of cancer that is highly prevalent in Indian populations.
Lung, breast, colon and prostate cancers occur commonly in developed countries. However, gallbladder cancer (GBC) is largely an “Indian Cancer”, prevalent in northern India and rare in the west, resulting in limited treatment strategies. The survival rate in advanced stage patients is less than 15%.
Conventional therapy for cancers usually involves chemotherapy and radiation. Chemotherapy consists of a “chemical poison” administered intravenously at a dosage where the patient survives, but the cancer dies. In the process, the drug ends up killing many normal cells, reducing the quality of patient’s life. Major side effects include loss of hair, damage to cells in the bone marrow, mouth, digestive tract and reproductive system.
Instead, personalised therapy aims to target the cancerous cells specifically, leaving the normal cells unharmed. “Personalised therapy endeavours to treat cancer compassionately with an oral pill similar to other chronic diseases like Diabetes,” says Dutt.
The researchers collected early-stage gallbladder tumour samples from patients and performed high throughput genome-wide analysis to detect genetic abnormalities in these cells. The researchers found that a number of genes that are associated with the EGFR signalling pathway were mutated or dysregulated in a large proportion of tumour samples. The EGFR pathway plays an important role in cell growth, proliferation and survival and is implicated in various cancers.
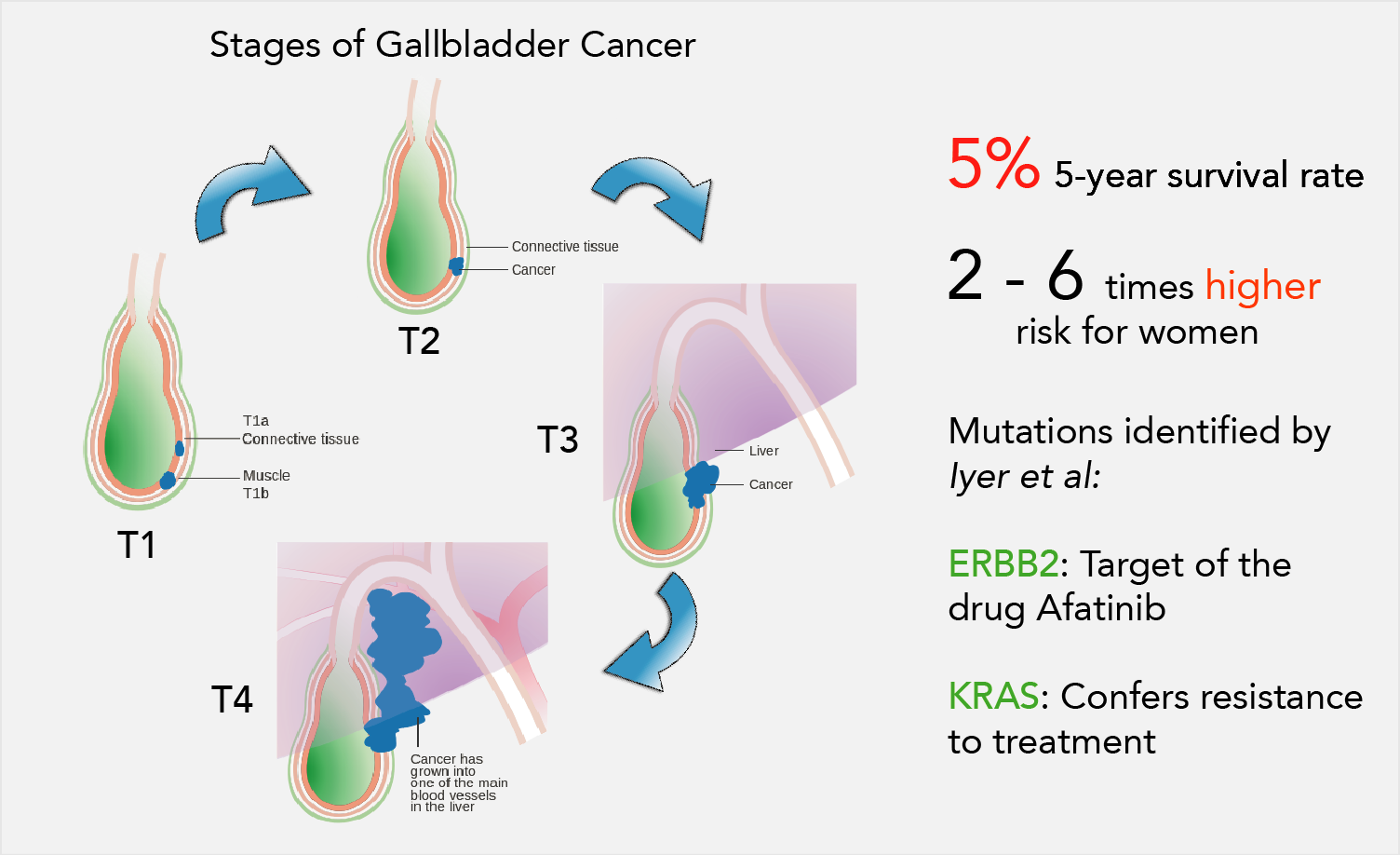
Amongst the genes showing aberrant expression in tumour cells, two that attracted the researchers’ interest were ERBB2 and KRAS. ERBB2 is overexpressed in a number of breast cancers, and more importantly, it is druggable, which means that its activity can be inhibited by approved drugs used to treat other cancer types.
The researchers found that inhibiting or blocking ERBB2 activity in gall bladder tumour cell lines decreased survival of these cells, but not when KRAS was mutated as well. This indicates that the presence of the KRAS mutations renders the tumour cells resistant to therapy targeting ERBB2 and its downstream signalling. These results agree with a similar clinical algorithm known in colorectal cancer, where the occurrence of KRAS mutation was routinely monitored and if detected the patients were precluded from anti-EGFR therapy.
“This research suggests that tumours with additional genomic alterations may lead to patient-specific drugs,” says Prajish Iyer, the first author of the study. Based on this study, a case can be made for KRAS mutation profiling of gallbladder cancer patients, which may allow the clinicians to quickly predict and identify patients who would be responsive or non-responsive to treatment.
ERBB2 is a known target of the drug Afatinib, an EGFR inhibitor. Afatinib has shown remarkable promise in the treatment of cancer in previous clinical trials. However, an inadequate number of gallbladder cancer patients is a major impediment to recruit patients for a conventional clinical trial to test Afatinib’s efficacy.
Based on the findings from this study, gallbladder patients can instead be recruited under a newer generation “basket clinical trial” for Afatinib. In these trials, instead of enrolling patients based on the organ of origin of the tumour (gallbladder, lung, cervix etc.), patients of any tumour type having common molecular mutations such as ERBB2 are recruited.
“The plan would be to validate our findings in a larger cohort and fast track the process into human clinical trials,” says Shailesh V. Shrikhande, Head, Division of Cancer Surgery, Tata Memorial Hospital, Tata Memorial Centre, Mumbai, and an author on the paper.
Did you enjoy this article? Please let us know in the comments below.